What is Critical Care
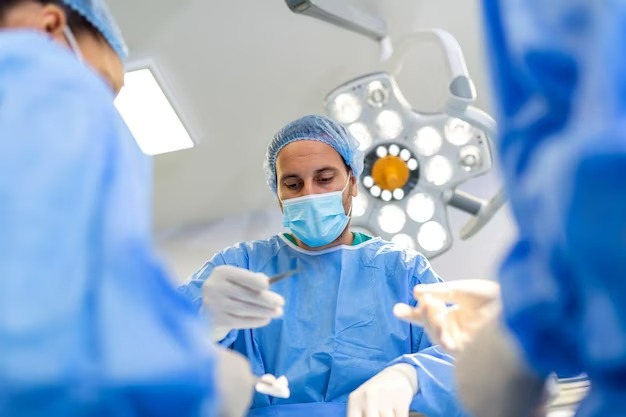
Critical care (also known as Intensive Care) is a multiprofessional healthcare specialty that cares for patients with acute, life-threatening illnesses or injury. Illnesses or injury not uncommonly can endanger life and in such situations several organs in the body need rigorous monitoring and management. Emergent care can be provided wherever life is threatened – at the scene of an accident, in an ambulance, in a hospital emergency room, or in the operating room. However, critical care today is delivered in highly specialized units called intensive care units (ICU). Various terminologies like Multidisciplinary Critical Care Unit (MDCCU), Critical Care Unit (CCU), Intensive Medical Care Unit (IMCU), Intensive Therapy Unit (ITU), Coronary Care Unit (CCU) may be used to describe such services in a hospital. Such intensive care warrants timely, diligent, multi-disciplinary and co-ordinated care of multiple medical problems simultaneously in a patient to ensure recovery and return to baseline function.
Critical care is provided by multidisciplinary teams of highly experienced and professional physicians, nurses, respiratory care technicians, physiotherapists, dieticians, pharmacists and other allied health professionals. The team members use their unique expertise, ability to interpret complex and important therapeutic information, access to highly sophisticated equipment and the services of support personnel to provide care that leads to the best outcome for the patient.
Patients are rarely admitted directly to the critical care unit. Rather, they are usually admitted from the emergency room, or surgical area where they are first given care and stabilized. The continuum of critical care begins at the moment of illness or injury and continues throughout the patient’s hospitalization, treatment and subsequent recovery.
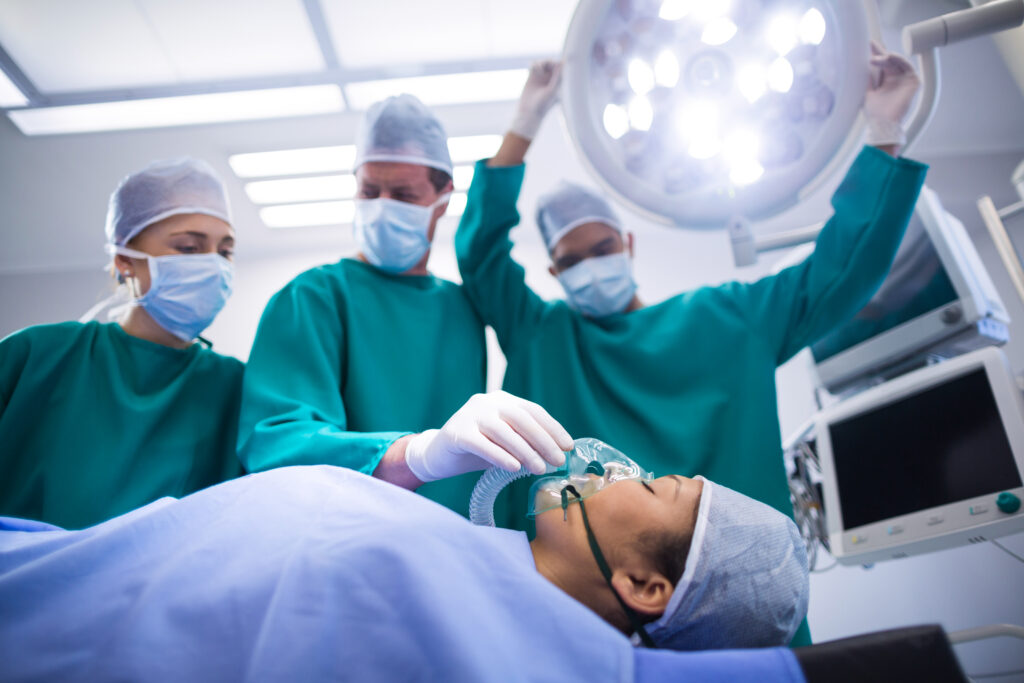
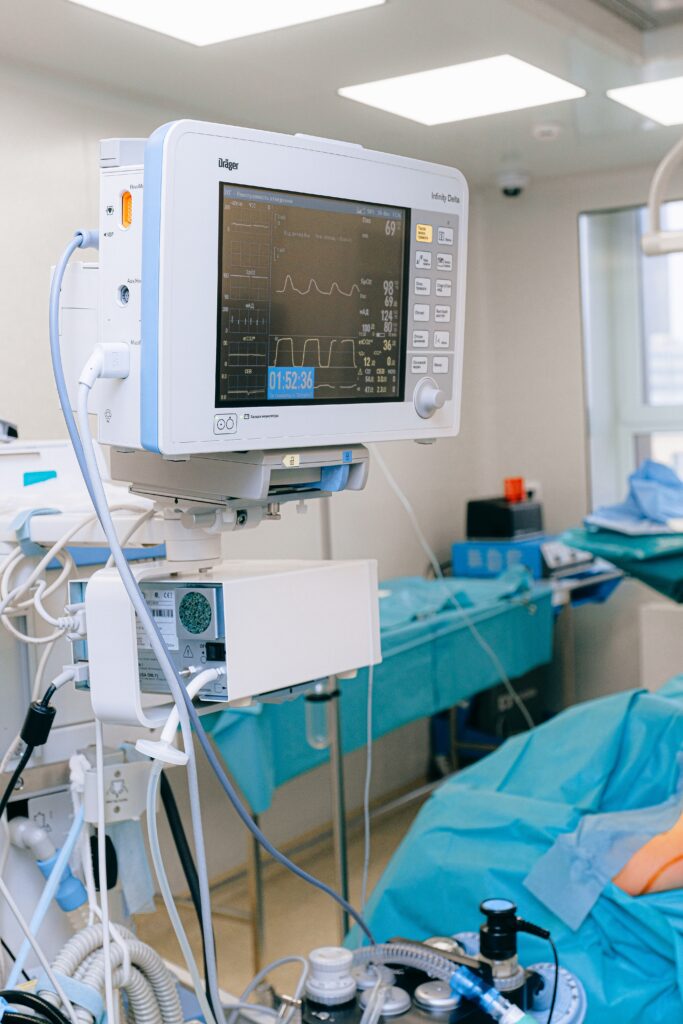
Is Critical Care a new medical specialty?
Critical care evolved from an historical recognition that the needs of patients with acute, life-threatening illness or injury could be better treated if they were grouped into specific areas of the hospital. Nurses have long recognized that very sick patients receive more attention if they are located near the nursing station. Florence Nightingale wrote about the advantages of establishing a separate area of the hospital for patients recovering from surgery.
Intensive care began in the United States when Dr. W.E. Dandy opened a three-bed unit for postoperative neurosurgical patients at the Johns Hopkins Hospital in Baltimore. In 1927, the first hospital premature-born infant care center was established at the Sarah Morris Hospital in Chicago. During World War II, shock wards were established to resuscitate and care for soldiers injured in battle or undergoing surgery.
In 1947-1948, the polio epidemic raged through Europe and the United States, resulting in a breakthrough in the treatment of patients dying from respiratory paralysis. In Denmark, manual ventilation was accomplished through a tube placed in the trachea of polio patients. Patients with respiratory paralysis and/or suffering from acute circulatory failure required intensive nursing care. During the 1950s, the development of mechanical ventilation led to the organization of respiratory intensive care units (ICUs) in many European and American hospitals. The care and monitoring of mechanically ventilated patients proved to be more efficient when patients were grouped in a single location. General ICUs for very sick patients, including postoperative patients, were developed for the similar reasons. Between 1990 and the present, critical care significantly reduced in-hospital time as well as costs incurred by patients with diseases such as cerebrovascular insufficiency and lung tumors.
The development of new and complicated surgical procedures, such as transplantation of the liver, lung, small intestine, and pancreas, created a new and important role for critical care following transplantation.
Widespread utilization of non-invasive patient monitoring has further reduced the cost and medical/nursing complications associated with care of critically ill and injured patients. Ubiquitous availability and use of pharmacologic therapy for critical care patients with specific organ system failure has reduced time spent in both critical care units and in the health care facility.
Most frequently asked questions
Any illness or injury that potentially threatens life warrants critical care. Typical examples of critical illness include heart attack, poisoning, pneumonia, surgical complications, premature birth, and stroke. Critical care also includes trauma care – care of the severely injured – whether due to an automobile accident, gunshot or stabbing wounds, a fall, burns, or an industrial accident.
Critical care refers exclusively to the treatment of patients who suffer from life-threatening conditions. Emergency room physicians and nurses treat patients who suffer from minor emergencies (sprained ankles, broken arms) to those with major problems including heart attack, knife or gunshot wounds or drug overdoses. In the Emergency Department, physicians and nurses stabilize patients and transport them to the ICU or other area of the hospital for further treatment. The long-term management of critically ill and injured patients is provided by critical care professionals in the ICU.
An intensivist (also known as Critical Care Specialist) is a doctor with subspecialty training, or equivalent qualifications, in critical care. An intensivist directs the care of critically ill and injured patients and works in collaboration with other health care professionals necessary for the care of patients in critical care units.
A registered dietician is a vital part of the medical team that consults with physicians, nurses, therapists, and family members in the ICU. The registered dietician works to improve the nutritional health and promotes recovery of the critical care patient.
A social worker is a licensed professional that works with the ICU interdisciplinary team to provide a link between treatment plans for the critical care patient and family members. Special knowledge that is acquired through formal, professional social work education, welfare policies and services, and social welfare systems and community resources guide the practice of social work.
Respiratory therapists work with the critical care team to monitor and promote airway and respiratory management of the critical care patient. This may include: oxygen therapy, aerosol medication therapy, cardio-respiratory monitoring, mechanical ventilation (breathing machine) management and patient and caregiver education.
The critical care team includes a diverse group of highly trained professionals who provide care in specialized care units and work toward the best outcome possible for seriously ill patients. All members of the team may be asked to teach patients and their families various strategies to improve health, healing, coping, and well-being specific to their area of expertise. Although the members could vary between hospitals, an optimal team would include:
Physicians who have primary qualification in a medical specialty, such as surgery, internal medicine, pediatrics, or anesthesiology, and who also receive higher education, training, and subspecialty certification in critical care. Intensivists are generally assigned to the ICU on a full-time basis and work with other critical care team members to provide their patients with ongoing and consistent care. These physicians know how specific treatments affect all the organ systems, avoid duplication of procedures and medications, and honor the patient’s preferences regarding medical treatment as well as End of Life care (when appropriate). Intensivists may also coordinate the administrative environment of the ICU by setting policies, developing protocols, and facilitating communication among primary care physicians, specialists, patients, and their families.
Critical care nurses provide a high level of skilled nursing for total patient care and often facilitate communication between all of the people involved in the care of the patient. Their expertise and continuous presence allows for early recognition of subtle, but significant, changes in patient conditions, thereby preventing worsening conditions and minimizing complications that arise from critical illness. Because of their close contact with the family and the patient, critical care nurses often serve as the patient’s advocate and become integral to the decision-making process of the patient, family, and critical care team.
A clinical pharmacologist is a certified specialist in the science and clinical use of medications. Patients in ICU often have special needs in titration of their medications in view of their organ failures. The pharmacist with specialty training in the ICU is equipped in recognizing these needs and problems and work with members of the health-care team to foster effective and safe medication therapy.
The physical therapist provides services that restore function, improve mobility, relieve pain, and prevent or limit permanent physical disabilities. The occupational therapist is trained to make a complete evaluation of the impact of the disease on the daily activities of the critical care patient at home, in work situations, and recreational activities. Both members work cooperatively with other disciplines of the healthcare team to reduce physical and psychological disability of the patient.
Your primary physician is an important link between the critical care team and the patient and family. The primary physician has a complete medical history of the patient, is often a trusted confidante of the family and may be aware of the patient’s values, attitudes and health care preferences. Critical care teams often work closely with the primary physician to determine pre-existing illness, allergies, use of medications, and other factors which may influence the health of the patient.
